|
7/27/2023 0 Comments Blowout fracture
INTRODUCTION This topic will review the evaluation and management of patients with orbital fractures, mechanisms of injury to the orbit, fracture types, and associated injuries. Rarely fragments from an orbital floor fracture buckle up into the orbit, an injury referred to as a "blow-in" fracture. blowout fracture of the orbit direct impact on the orbit may elevate orbital pressure sufficiently as to fracture the thin medial and inferior walls the. Michael Ganetsky, MD Literature review current through: Mar 2023. Surgery is rarely needed for medial wall fractures. The treatment of pure orbital blow-out fractures is often conservative but orbital floor repair may be necessary if there are complications such as inferior rectus muscle compromise. In the supine position, fluid and debris in the maxillary antrum can layer against the orbital floor and obscure soft tissue herniating through the fracture.For those patients in whom direct coronal scans are not possible (for example due to other injuries or if the patent is unable to co-operate), axial CT scans with coronal reconstructions are an alternative method of imaging, particularly with the use of multidetector CT. Direct coronal CT scans (with the patient prone) are best for demonstrating blow-out fractures. 
A CT scan is indicated if there is diplopia or restriction of eye movements, and to assess the extent of the injury. Mild or transient diplopia can occur simply due to the periorbital oedema or haemorrhage. If the inferior rectus muscle or its sheath herniates through the fracture and becomes trapped, it may be compromised resulting in diplopia on looking down or straight ahead. 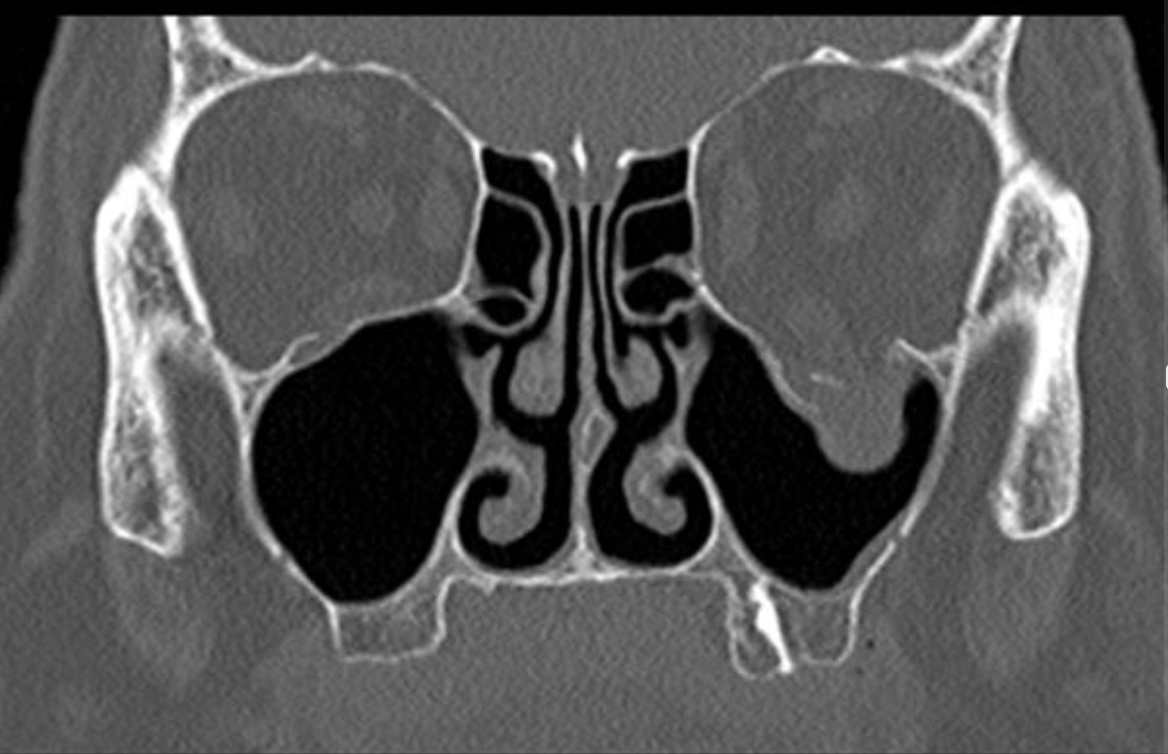
The fracture fragments are rarely demonstrated on plain films. Blow-Out Fractures What causes a Blow-Out Fracture An orbital fracture is typically caused when a fist or ball strikes the eye. An air-fluid level may be seen in the maxillary sinus. Other signs of a blow-out fracture are air within the orbit (which has entered from the maxillary or ethmoid sinuses), an indistinct orbital floor on occipitomental views and opacification of the sinuses due to blood within them. Orbital floor fractures may result when a blunt object, which is of equal or greater diameter than the orbital aperture, strikes the eye. This appearance has been likened to an opaque tear drop hanging from the roof of the antrum and may be the only radiographic evidence of a blow-out fracture. On occipitomental (facial) x-rays this is seen as a convex mass projecting into the roof of the right maxillary sinus. Orbital contents may then herniate downwards through the orbital floor fracture into the maxillary sinus. The orbital rim remains intact in pure blow-out fractures. These are the thin plates of bone that form the orbital floor (roof of the maxillary antrum) and the medial wall of the orbit (lateral wall of the ethmoid sinuses). There is an acute increase in intraorbital pressure which is relieved by fracture through the weakest parts of the orbit. His one great achievement is being the father of three amazing children.A blow-out fracture of the orbit results from a direct compressive force to the eye, e.g. He is one of the founders of the FOAM movement (Free Open-Access Medical education) and is co-creator of , the RAGE podcast, the Resuscitology course, and the SMACC conference. He created the ‘Critically Ill Airway’ course and teaches on numerous courses around the world. He coordinates the Alfred ICU’s education and simulation programmes and runs the unit’s education website, INTENSIVE. He is actively involved in in using translational simulation to improve patient care and the design of processes and systems at Alfred Health. He has completed fellowship training in both intensive care medicine and emergency medicine, as well as post-graduate training in biochemistry, clinical toxicology, clinical epidemiology, and health professional education. He is an internationally recognised Clinician Educator with a passion for helping clinicians learn and for improving the clinical performance of individuals and collectives.Īfter finishing his medical degree at the University of Auckland, he continued post-graduate training in New Zealand as well as Australia’s Northern Territory, Perth and Melbourne. He is on the Board of Directors for the Intensive Care Foundation and is a First Part Examiner for the College of Intensive Care Medicine. He is also a Clinical Adjunct Associate Professor at Monash University. He is a co-founder of the Australia and New Zealand Clinician Educator Network (ANZCEN) and is the Lead for the ANZCEN Clinician Educator Incubator programme. Chris is an Intensivist and ECMO specialist at the Alfred ICU in Melbourne.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
